LCL Repair& Reconstruction
Restoring lateral joint stability and treating complex PLC injuries.
LCL Repair & Reconstruction
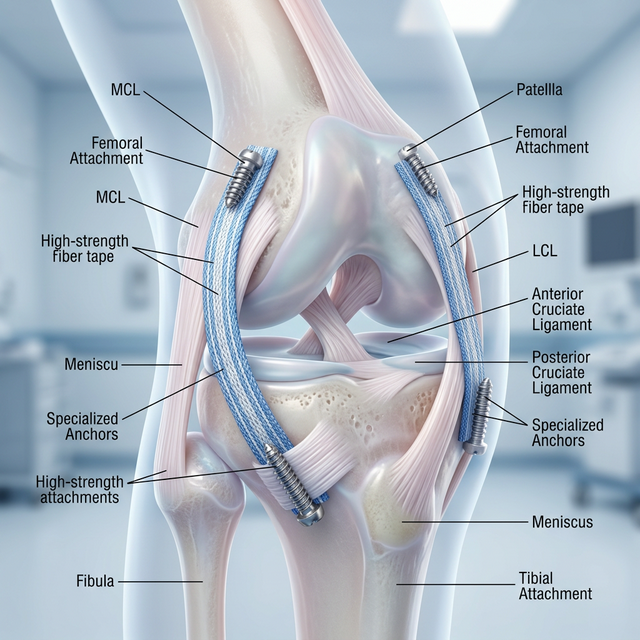
The Lateral Collateral Ligament (LCL) is a critical anchor on the outside of the knee, responsible for preventing abnormal outward bowing (varus stress). Injuries to the LCL are often combined with damage to the Posterolateral Corner (PLC)—a complex of tendons and ligaments that provide rotational control. Dr. Ravi Teja utilizes advanced anatomical reconstruction techniques, using either autografts or high-strength allografts, to rebuild these structures. Precise tunnel placement and graft tensioning are essential to restore a natural feel to the knee and prevent the early onset of lateral compartment arthritis.
Surgical Process
Rotational Audit
Using the dial test and stress-radiographs to identify the degree of lateral and rotational laxity.
Anatomical Rebuild
Creating precise bone tunnels in the femur and fibula that mirror the original FCL footprint.
Graft Fixation
Securing the new lateral pillar with specialized interference screws for immediate mechanical stability.
Patient Care
Recovery Roadmap
Recovery is gradual, typically requiring a protective range-of-motion brace for 6-8 weeks. Patients use crutches for 2-4 weeks to protect the new lateral pillar. Return to pivoting and high-impact sports takes 6-12 months.
Who Needs This Procedure?
Patients with significant 'varus' instability (knee bowing outward) after an injury
Individuals who feel their knee 'gives way' when pushing off or changing direction
Patients with LCL tears combined with other ligament injuries (ACL or PCL)
Athletes needing anatomical reconstruction to return to high-impact sports
Clinical Results & Gallery
Procedural Intelligence
Elite Patient Care
Dr. Ravi Teja provides personalized evaluations using the latest diagnostic technology for LCL Repair & Reconstruction.
Book EvaluationElite Standard
Certified Excellence
Safety First
Minimal Complications